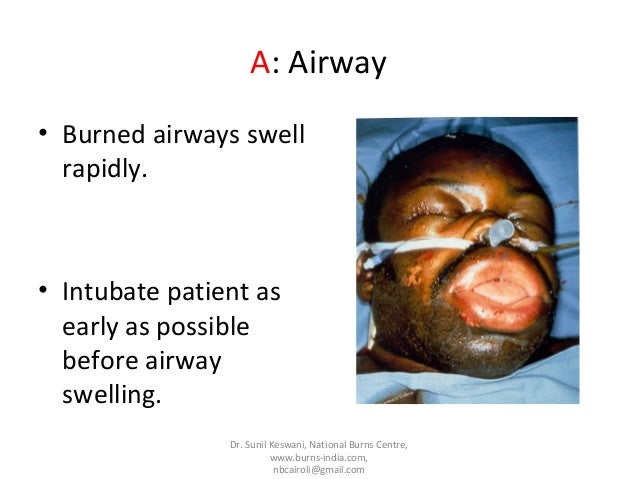
Burn Patients Intubation
Key points.Maintain a high suspicion of smoke inhalation in a flame injury.Initial resuscitation priorities are administration of 100% oxygen and early intubation with an uncut tracheal tube if airway at risk.Utilize lung-protective ventilation strategies and consider early bronchoscopic washout.Administer careful fluid therapy to avoid over/under-resuscitation.Remember to consider cyanide poisoning as early use of antidote improves outcome.DefinitionSmoke inhalation injury can be defined as damage caused by breathing in harmful gases, vapours, and particulate matter contained in smoke. It can manifest as a thermal injury, chemical injury, and as systemic toxicity, or any combination of these. EpidemiologyMost burns managed in hospitals are from scalds (54%) and contact burns (23%). Patients with thermal injury from fires and explosions, who are more likely to have smoke inhalation injury, represent only 16% of the total. The pathophysiological sequelae of breathing in smoke are life-threatening and multi-systemic.Smoke inhalation is present in 2–30% of all flame burns presentations and in higher proportions if facial burns are present. It has a high mortality associated with it and is the most common cause of death at the scene of a fire.
The presence of a smoke inhalation injury, alongside patient age and percentage of body surface area burned, is a major determinant of mortality. Inhalation injury increases the risk of death from a burn injury 3.6-fold. Smoke inhalation injury leads to respiratory complications in 73% and acute respiratory distress syndrome (ARDS) in 20%.Burns are an injury process of vulnerable populations. Age is an important predictor, with older (64 yr) and younger (20% and smoke inhalation injury meet the national criteria for referral to a Burns Centre. Respiratory supportA severe chest burn may require escharotomy. This should be considered if there are restricted chest movements with a full thickness circumferential chest burn.
This may present as decreasing tidal volumes requiring higher inspiratory ventilator pressures. Of note, especially in children, a deep burn to the anterior chest and abdomen may compromise respiratory function in the absence of a circumferential burn.Intubated patients should undergo fibreoptic bronchoscopy to diagnose and grade inhalation injury. The severity does correlate with long-term prognosis, although the best predictor is the P a O 2 / F I O 2 ratio.
Practice Essentials. Burn care should begin at the site of injury and continue through prehospital care and transportation to the closest burn center, or to the closest emergency department (ED) with advanced life support capability, followed by transfer to a burn center when appropriate. The image below depicts partial- and full-thickness burns.
Moreover, the evidence suggests improved outcomes with bronchoscopy and early clearance of particulate matter and washout.Lung-protective ventilatory strategies limiting tidal volumes to 6 ml kg −1 predicted body weight, the application of PEEP, and permissive hypercapnia have been adopted from the ARDS population. There is limited evidence in victims of smoke inhalation that these techniques limit atelectasis and barotrauma, but it is a common sense strategy to avoid ventilator-induced lung injury in these at-risk patientsA regimen of aerosolized heparin alternating with a solution of 20% acetylcysteine was studied on paediatric and adult populations with inhalation injury diagnosed on bronchoscopy. Acetylcysteine is a mucolytic agent, and hence should diminish airway cast formation. Heparin is a potent activator of anti-thrombin III, and so leads to thrombin inactivation and also decreases airway casts. One retrospective case–control study found a significantly decreased mortality, occurrence of atelectasis, and need for re-intubation in the treatment group (class III evidence). In a small single-centre study in adults, it was found the nebulized therapy attenuated lung injury and progression of ARDS compared with historical controls. There are reports of experience using nebulized heparin in Burn Centres in the USA, UK, and Singapore, but there are no large trials to support widespread adoption.
An example of an inhalation protocolThe doses of heparin and acetylcysteine below are suitable for adults and children. Heparin and acetylcysteine should be alternated, so patients receive treatment every 2 h.There is no place for prophylactic antibiotics. Patients with inhalation injury do have increased risk for secondary bacterial infection, most commonly Staphylococcus aureus and Pseudomonas aeruginosa. However, the use of prophylactic antibiotics promotes the emergence of resistant organisms.Nebulized heparin 5000 IU diluted with 3 ml 0.9% saline 4 hourly for 5 days.Nebulized 20% acetylcysteine solution, 3 ml every 4 h. This may be irritant to the airway and should be discontinued if new bronchospasm develops or existing bronchospasm worsens.Nebulized salbutamol 2–4 hourly.Chest physiotherapy and regular respiratory toilet are essential.Steroids are not recommended in the treatment of inhalation injury but may have a role in preventing post-extubation stridor caused by laryngeal oedema, although there have been no specific studies in burn patients. Ventilator care bundlePatients with smoke inhalation injury are at high risk for ventilator-associated pneumonia and standard preventive measures should be instituted where possible.
Cardiovascular supportAdequate support, initially by fluids then pharmacological means as appropriate, should be utilized to minimize tissue hypoxia. There are no data on therapeutic hypothermia for pre-hospital arrest in this patient group.The Parkland formula (Table ) is the most frequently used burn resuscitation formula applied to guide initial fluid management.
Formulas should not be followed blindly, but fluid infusions should be adjusted to clinical response. Smoke inhalation patients have higher fluid requirements for the same size burn, which may be up to 40% greater. This should be balanced against the attendant risks of pulmonary oedema and worsening capillary leak.
Use cardiac monitoring early if available. Avoid large fluid volumes aiming to either correct any base deficit or target urine output in excess of 0.5 ml kg −1 h −1. Parkland formula for burn resuscitationVolume4 ml×% burn×person's weight in kgFluidCompound sodium lactate (Hartmann's solution)TimingHalf of this total volume should be administered over the first 8 h, with the remainder given over the following 16 h. It is important to note that this time frame is calculated from the time at which the burn is sustained, and not the time at which fluid resuscitation is begunWhenGiven to burns 10% in children and 15% in adultsMaintenanceChildren. Parkland formula for burn resuscitationVolume4 ml×% burn×person's weight in kgFluidCompound sodium lactate (Hartmann's solution)TimingHalf of this total volume should be administered over the first 8 h, with the remainder given over the following 16 h.
It is important to note that this time frame is calculated from the time at which the burn is sustained, and not the time at which fluid resuscitation is begunWhenGiven to burns 10% in children and 15% in adultsMaintenanceChildren. Parkland formula for burn resuscitationVolume4 ml×% burn×person's weight in kgFluidCompound sodium lactate (Hartmann's solution)TimingHalf of this total volume should be administered over the first 8 h, with the remainder given over the following 16 h. It is important to note that this time frame is calculated from the time at which the burn is sustained, and not the time at which fluid resuscitation is begunWhenGiven to burns 10% in children and 15% in adultsMaintenanceChildren.
Parkland formula for burn resuscitationVolume4 ml×% burn×person's weight in kgFluidCompound sodium lactate (Hartmann's solution)TimingHalf of this total volume should be administered over the first 8 h, with the remainder given over the following 16 h. It is important to note that this time frame is calculated from the time at which the burn is sustained, and not the time at which fluid resuscitation is begunWhenGiven to burns 10% in children and 15% in adultsMaintenanceChildren. Investigations Laboratory studies.Full blood count.Urea and electrolytes.Arterial blood gas.Lactate levels.Carboxyhaemoglobin (COHb) level.Arteriovenous oxygen difference (a reduced level implies inability to utilize oxygen).BronchoscopyGold standard diagnosis is by bronchoscopy, reported to be 86% accurate. Bronchoscopic findings consistent with inhalation injury include carbonaceous debris and mucosal pallor, ulceration, or erythema. Pulmonary toilet with washout may lessen the injury.
Washout fluid can be sent for microscopy and culture. There is no conclusive evidence on the timing and benefit of serial bronchoscopy, although one retrospective study did suggest a slight improvement.
RadiologyChest X-ray may be normal, although may later show signs of diffuse atelectasis, pulmonary oedema, or bronchopneumonia. Carbon monoxide poisoningAssuming carbon monoxide (CO) poisoning in all fire victims is prudent.
Standard pulse oximetry will not distinguish COHb from deoxygenated or oxygenated haemoglobin and so overestimates oxygen saturations. Low COHb levels in the emergency department do not exclude significant CO exposure, as timely application of high flow oxygen at the scene will cause rapid washout.Features of severe poisoning:.Any new objective acute neurological signs, for example, increased muscle tone, up-going plantars.Coma.ECG indication of ischaemia.Clinically significant acidosis.Initial COHb levels 30%.TreatmentAdminister high-flow oxygen via a non-rebreathing mask, unless intubated then ventilate the lungs with F I O 2 1.0.
Intensive care unit (ICU) admission including mechanical ventilation is likely to be required in cases of severe poisoning. The UK National Poisons Information Service (NPIS) does not currently recommend hyperbaric oxygen therapy in the context of smoke inhalation injury. Hydrogen cyanide poisoningThere is a risk of exposure to cyanide after smoke inhalation, particularly from fires involving synthetic materials (e.g. Furnishings, plastics, vinyl). Such patients are often hypoxic and exposed to carbon monoxide making the diagnosis of cyanide toxicity more complicated.Cyanide (CN) levels are not readily available (currently, only UK laboratory measuring cyanide levels is in Cardiff), so treatment should not wait for levels.
The following suggest cyanide poisoning:Severe toxicity features:.lactate 7 mmol litre −1,.elevated anion gap acidosis,.reduced arteriovenous oxygen gradient.Headache, confusion, convulsions, loss of consciousness, fixed unreactive pupils.Arrhythmias, myocardial ischaemia and cardiovascular collapse.TreatmentImmediate management should include high-flow oxygen and supportive ICU care. NPIS can provide advice on the use of specific antidotes. If metabolic acidosis persists despite correction of hypoxia and adequate fluid resuscitation, consider correction with i.v. Sodium bicarbonate. Rapid correction is particularly important if there is prolongation of the QRS or QT intervals.
AntidotesConsider treating burns patients with a good history of smoke inhalation injury who have arterial blood lactate concentration 10 mmol litre −1 (indicative of moderate-to-severe poisoning) in the absence of significant burns and after correction of hypotension; a history of loss of consciousness; cardiovascular instability; or cardiac arrest.If the patient has significant burns and smoke inhalation, clinical judgement must be used to assess the adequacy of resuscitation before attributing elevated lactate to cyanide poisoning. Cardiac output monitoring should be considered. Remember antidotes have side-effects. There are no data available on the length of time that antidotes are effective for after cyanide exposure.
Hydroxocobalamin (Cyanokit ®)Hydroxocobalamin is probably the safest antidote for patients with concomitant smoke inhalation and burns. It works by binding to HCN to form non-toxic cyanocobalamin, which is then excreted by the kidneys. In France, this has been used in the pre-hospital setting for the last 10 years.
It should be given as early as possible after smoke exposure where cyanide toxicity is suspected and given immediately if in cardiac arrest.Adult dose: 5 g over 15 min, may be repeated×1, given over 15 min–2 h.Paediatric dose: 70 mg kg −1 over 15 min (not exceeding 5 g); may be repeated once to max 140 mg kg −1, given over 15 min–2 h, maximum dose 10 g.Like all cyanide antidotes, hydroxocobalamin has side-effects, but these are usually not problematic. The most noticeable is the reddish brown skin, mucous membranes (up to 15 days), and urine discoloration (can last up to 35 days). This discoloration can affect colorimetric laboratory blood tests and can trigger false ‘blood in line’ alarms on haemofiltration machines. It can cause false elevation COHb level on co-oximetry (∼5% increase) and transient hypertension which may be beneficial in hypotensive patients.
Anaphylaxis reactions are rare. Other antidotes.Amyl and sodium nitrites induce methaemoglobin, which combines with cyanide. This will further limit oxygen delivery, so should be avoided in smoke inhalation injury, especially if COHb 10%. Also can cause severe hypotension from vasodilation.Dicobalt edetate is toxic and potentially fatal in the absence of cyanide poisoning due to cobalt toxicity. Use only if poisoning is confirmed and is severe.Sodium thiosulphate enhances the conversion of cyanide to thiocyanate, which is renally excreted (delayed effect and is used with other antidotes with faster action). Co-administration with hydroxocobalamin may be beneficial.ConclusionSmoke inhalation injury is a serious injury with a high associated mortality and morbidity. Early recognition and prompt management are critical.
Treatment is predominantly supportive and avoiding iatrogenic complications. There are some recognized treatments for the pulmonary injury and the systemic toxicity, and the subject is being researched for new potential options to modulate the inflammatory response and limit cast formation.
In view of the complexity of the injury and the dynamics of the pathophysiology, it is likely that treatment modalities will be multi-targeted. Declaration of interestNone declared.
Key points.Crystalloid is the fluid of choice for resuscitation, volume calculated by the Parkland formula=4 ml kg −1 (%burn) −1.Hypovolaemic shock in the first few hours after a burn injury is never due to the burn alone.Primary and secondary survey should follow ATLS principles (do not get distracted by the burn).Blood loss during debridement and grafting can be significant and insidious.Major burns require a dedicated multidisciplinary team for adequate management.Major burns are systemic injuries requiring input from multiple specialities. There are ∼140 000 cases of new burns per year presenting to emergency departments in England and Wales, with around 10% of these being admitted to hospital. Of these, 4000–5000 cases are complex and require the services of a regional adult burns unit.
The majority of the others will be managed by hospitals with a plastic surgery service.Important considerations in the clinical outcome for these patients are early resuscitation, multidisciplinary team management, early surgical debridement, and prevention of complications. Anaesthesia in this group of patients can be challenging with profound hypermetabolism, pain management issues, alteration of drug pharmacokinetics, potential airway problems, temperature control, and substantial blood loss.Overall, the mortality rate among hospitalized burn patients in a recent review of European data was 13.9% (4–28.3%).
Major risk factors for death are older age, a higher total percentage of burned surface area, inhalation injury mortality rate 27.6% (7.8–28.3%), and chronic diseases. There appears to be no sex-related difference in survival after thermal injury.
Multi-organ failure and sepsis are the most frequently reported causes of death. The main causes of early death (40%, or patients failing to respond to conventional therapy.
Patients with HbCO levels 25–30% should be ventilated.Cyanide poisoning should be suspected in burn patients with an unexplained and persistent lactic acidosis, despite adequate fluid resuscitation. BreathingBreathing, chest movement, and tracheal position should be assessed clinically. There are several ways that a burn injury can compromise respiration. Mechanical restriction of breathingDeep dermal or full-thickness circumferential burns of the chest may severely restrict chest wall movement and relieving escharotomies may be necessary to allow adequate ventilation.
These are rarely, if ever, needed before admission to a burn service. Blast injuryPenetrating injuries can cause tension pneumothoraces, and the blast itself can cause lung contusions and alveolar trauma which may lead to adult respiratory distress syndrome. CirculationTwo large-bore i.v. Cannulae should be inserted through the unburnt skin if possible and baseline bloods sent. Traditional sites for i.v. Access may be unavailable and unusual peripheral venous sites or central venous access is required (usual indications for central venous line insertion also apply).
The groins are usually spared so femoral venous cannulation is often possible. Burns are not the cause of immediate hypovolaemia.
If there are features of hypovolaemic shock, the patient is almost certainly bleeding from other injuries. Warmed Hartmann's solution should be started and titrated to cardiovascular signs, but if stable can be run slowly until the burn calculation is made (see the Exposure and estimation and Fluids sections). DisabilityA brief assessment of the conscious level should be made using the GCS score and pupils examined. Exposure and estimationExpose and ensure all jewellery and watches are removed from burnt limbs. The patient should be examined (including the back—log roll if appropriate) to get an accurate estimate of the burn area and to check for any concomitant injuries. Burn patients become hypothermic easily, so should be covered and warmed as soon as possible.
Burns are classified by total body surface area (TBSA) and depth. A standard Lund–Browder chart is readily available in most emergency departments for a quick assessment of BSA burnt. If this is not available, the ‘Rule of Nines’ is fairly accurate in adult patients (Fig. ). Wallace Rule of Nines. Reproduced from: Hettiaratchy S, Papini R. Initial management of a major burn: II—assessment and resuscitation.
Br Med Jnl 2004; 329: 101–3. With permission from BMJ Publishing Group Ltd. Fluid resuscitation is required in adults if the burn involves more than 15% BSA or 10% with smoke inhalation.
The Parkland formula is the most widely used resuscitation guideline and is 4 ml kg −1 (%burn) −1 which predicts the fluid requirement for the first 24 h after the burn injury. Starting from the time of burn injury (not time of presentation), half of the fluid is given in the first 8 h and the remaining half is given over the next 16 h. The fluid of choice is Hartmann's solution. Any fluid already given should be deducted from the calculated requirement. A urinary catheter should be inserted and hourly urine output is a used as a guide to resuscitation.
In adults, at least 0.5 ml kg −1 h −1 should be passed. Example of calculation of fluid resuscitation in burnsA 32-yr-old man weighing 80 kg with a 30% flame burn was admitted at 23:00 h. His burn occurred at 22:00 h. He has already received 1000 ml of crystalloid from the emergency services.4 ml×(30% TBSA)×(80 kg)=9600 ml in 24 hWill receive 4800 ml during 0–8 h and 4800 ml during 8–24 h4800 (for first 8 h)–1000 (fluid already received)=3800 ml.Total fluid requirement for first 24 h.Half to be given in first 8 h, half over the next 16 h.Subtract any fluid already received and calculate hourly infusion rate for first 8 hBurn occurred at 22:00 h, so 8 h point is 06:00 h. It is now 23:00 h, so need 3800 ml over next 7 h.3800/7=543 ml h −1 from 23:00 to 06:00 hDivide figure in (ii) by 16 to give fluid infusion rate. Needs 4800 ml over 16 h:.Calculate hourly infusion rate for next 16 h4800/16=300 ml h −1 from 06:00 to 22:00 h the next day. AnalgesiaFull-thickness burns are painless; however, a mixed picture is common and the patient should receive i.v.
Morphine titrated against response.While all hospitals will be involved in the initial resuscitation of burn victims, complex burn injuries should be referred to and managed in a burns unit (Table ). If you are not sure whether a burn should be referred, discuss the case with your local burns unit. Anaesthesia and surgery for burnsInpatient burn injury care should be provided only by specialists trained in burn care in a burns unit. This is a reflection on the team approach to burn injuries, the resources, and infrastructure necessary to provide both critical care and the long-term management of the patient in terms of the planning and timing of surgical procedures.Recent trends in patient care have focused on early excision and wound coverage, aiming to remove the full-thickness injury and get biological closure.
This potentially reduces the risk of wound infection and the development of sepsis. The risk of this approach is the physiological insult of surgery to a patient who may well be deteriorating rapidly from their initial injuries. The most important and difficult clinical decisions are often made by the team at this stage. Escharotomy and decompressive therapiesThese are necessary when a number of factors come into play.
The patient will have a full-thickness circumferential burn resulting in an ‘eschar’ (from French eschare meaning scar or scab) which acts as a non-compliant tourniquet. When there is an additional insult from the accumulation of extracellular fluid as a result of resuscitation, there follows ischaemia and eventual necrosis of the affected compartment. Compartment pressures 40 mm Hg require decompression. Anaesthesia for wound debridement and graftingThe conduct of anaesthesia will be predicted by the TBSA, degree of systemic insult, and planned area for debridement and grafting. There is a trend towards earlier intervention and burn excision with the application of skin substitutes if donor skin is limited or further harvesting is not appropriate.Monitoring can be a challenge in major cases when access to chest (ECG), arms (arterial pressure), and digits (pulse oximetry) can be limited.
Skin staples or subcutaneous needles attached to crocodile clips can be used for ECG monitoring. Alternative sites for pulse oximetry such as the nose, lips, or tongue may be necessary. An arterial line is essential for major excisions and a cardiac output monitor can be useful. Blood loss can be significant and occasionally insidious. In major deep burns, we plan for 50–100 ml blood loss per% area excised, depending on the time post-burn (max 7–16 days) and the presence of infection.
This can often be compounded by thrombocytopenia and prolonged coagulation time which requires close liaison with haematology and blood bank.The patient will be hypermetabolic with a systemic inflammatory response (SIRS)-type cardiovascular system and often on vasoactive substances. This, combined with anaesthesia and significant blood loss, can make interpretation of haemodynamic changes quite taxing.These patients often require multiple anaesthetics/operations for dressing changes and grafting and pain management is difficult.
There is no evidence for improved outcome using TIVA vs inhalation anaesthesia and the technique used is an individual choice. With multiple anaesthetics, it is important to review the patient response to the previous event and adapt accordingly with the assumption that pain will be an escalating issue. Regional anaesthesia has a part to play but can be limited due to the large areas required to block and the risk of infection. Free frank sinatra songs download.
There needs to be a multimodal approach to analgesia in these patients with consideration given to the early use of neuropathic pain agents, such as pregabalin, and opioids and psychology input. Acute perioperative pain may need benefit from agents such as ketamine in addition to the usual analgesic ladder. The time taken for application of major dressings is another consideration, particularly with regard to temperature homeostasis.There are many preoperative anaesthetic considerations for burn wound excision/grafting (Table ).
PreoperativeIntraoperativePostoperativeAnaesthetic historyTemperature: hot theatre (32°C), fluid warmers, monitor—aim to lose. PreoperativeIntraoperativePostoperativeAnaesthetic historyTemperature: hot theatre (32°C), fluid warmers, monitor—aim to lose. PreoperativeIntraoperativePostoperativeAnaesthetic historyTemperature: hot theatre (32°C), fluid warmers, monitor—aim to lose. PreoperativeIntraoperativePostoperativeAnaesthetic historyTemperature: hot theatre (32°C), fluid warmers, monitor—aim to lose.
Critical care managementIn the first 24–48 h after resuscitation in patients with major burns, the hormonal response and inflammatory mediators cause hypermetabolism, immunosuppression, and SIRS. Fluid resuscitation and electrolyte managementThe fluid resuscitation aims to restore tissue perfusion avoiding end-organ ischaemia, preserving viable tissue and minimize tissue oedema. The Parkland formula is a guide and fluid resuscitation should be titrated against clinical response, invasive monitoring, and urine output (0.5 ml kg −1 h −1 in adults).
Invasive monitoring is necessary in the severely burnt patient to help guide both volume replacement and the use of ionotropes. The term ‘fluid creep’ describes the excessive volumes of fluid used for resuscitation which has occurred in some burn patients with complications (Table ). Hypokalaemia, hypophosphataemia, hypocalcaemia, and hypomagnesaemia are common and should be treated. There is a phenomenon known as ‘burn shock’ which describes a combination of hypovolaemic, distributive, and cardiogenic shock which is refractory to massive i.v. Experimental studies have looked at the use of hypertonic saline, high-dose ascorbic acid, or plasma exchange in this setting. Mechanical ventilationUsual lung protection strategies apply, and routine ventilator-associated pneumonia prevention strategies should be implemented.
Prophylactic corticosteroids or antibiotics have no role. In patients with inhalation injury, early tracheal intubation, aggressive pulmonary toilet, bronchodilator therapy, and bronchoscopic lavage are all important. HypothermiaPatients with large burns reset their baseline temperature to 38.5°C. This means that a patient with a core temperature of 37°C is relatively hypothermic. Strategies to prevent hypothermia include a warmed room (ambient temperature 28–32°C), warmed inspired air, warming blankets, and warmed fluids. This is also important to minimize the increase in basal metabolic rate caused by heat and evaporative water loss. Metabolism and nutritionThe increase in basal metabolic rate is proportional to the size of the burn and the presence of infection, peaking at 7–10 days.
This hypermetabolism can persist for up to 2 yr post-injury. Early enteral nutrition has been shown to improve survival in burn patients.
Meeting nutritional requirements (high protein, high carbohydrate feeds) is crucial to prevent protein breakdown, decreased wound healing, immune suppression, and an increase in infective complications. InfectionThis is a significant cause of mortality in major burns (Table ). Diagnosis of sepsis in burn patients is difficult as signs of SIRS induced by the burn are all normal findings, so regular microbiological surveillance is essential.